News
Members of the Beacon Bio team (from left) Eva Cai, Nicole Black, Dhrumi Gandhi, Melissa Castillo Bustamante, and Mischa Jurkiewicz. On May 5, Beacon Bio was named the $25,000 prize winner for the Health & Life Sciences Track in the 2021 Harvard President’s Innovation Challenge.
In the aftermath of the Boston Marathon bombing, one of the most prevalent injury survivors sustained was chronically perforated eardrums. Aaron Remenschneider, a surgeon and researcher at the Harvard-affiliated teaching hospital Massachusetts Eye and Ear (MEEI), helped treat many of these patients by performing tympanoplasties—surgeries to repair the ruptured eardrum using skin or cartilage from a different part of the body.
As he worked with these patients, Remenschneider dealt with the many pitfalls of tympanoplasty. For instance, the eardrum is never able to effectively regenerate after the procedure, often leading to poor hearing outcomes and in more than 50 percent of cases, revision surgery within five years.
These issues were top of mind when Remenschneider and his colleague Elliott Kozin met Nicole Black, Ph.D. ’20, then a graduate student at the Harvard John A. Paulson School of Engineering and Applied Sciences and Graduate School of Arts and Sciences. Black was working on 3D bioprinting projects in the lab of Jennifer Lewis, Hansjörg Wyss Professor of Biologically Inspired Engineering at SEAS and a Core Faculty member at the Wyss Institute for Biologically Inspired Engineering. They started discussing how 3D printing could be used to improve tympanoplasty outcomes while also decreasing the invasiveness of the procedure.
Six years later, Black, Lewis, Kozin, and Remenschneider are planning to co-found a startup, Beacon Bio, that seeks to create PhonoGraft, an eardrum graft from a novel, 3D-printed biomaterial that can eliminate many shortcomings of traditional tympanoplasty surgery.
On May 5, Beacon Bio was named the $25,000 winner for the Health & Life Sciences Track in the 2021 Harvard President’s Innovation Challenge.
“We studied whether we could fabricate these grafts using silicone or other off-the-shelf materials, but we soon realized that none of these materials were optimal,” Black said. “Your eardrum is an elastomeric tissue, so it is stretchy, but elastomeric materials, like silicone, don’t biodegrade. Thus, patients would have a piece of silicone in their eardrum forever putting them at risk of infection and biofilm formation. Instead, we set out to produce a biodegradable elastomer that we could 3D print.”
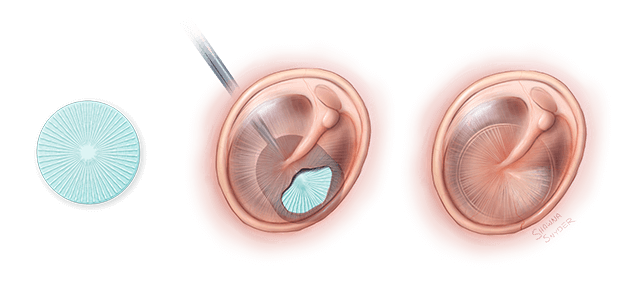
This illustration shows how the PhonoGraft (in blue) leads to functional and morphological regeneration of the tympanic membrane. (Illustration by Shawna R. Snyder)
Inspired by previous research on high-resolution polymer printing conducted in the Lewis Lab, Black spent much of her graduate studies designing an elastomeric ink that could be printed into complex architectures.
The biggest challenge of developing this material was creating a polymer that could be melt-extruded through the 3D printer, Black said. The research involved a great deal of back and forth—optimizing one element of the material changed other properties, so finding a balance took a lot of patience.
The material had to be printed into an extremely thin graft that would not crack when bent, but would still be able to degrade and support cell growth. Collaboration has been key to developing a product that will work in a clinical setting.
“From a surgical standpoint, the mechanical properties of a material are incredibly important. There are a number of labs around the world that have produced tissue scaffolds with very intricate designs, but without the ability to easily handle the grafts they can’t be used practically,” Remenschneider said. “Nicole invested considerable time to make sure that the graft exhibited properties that I need as a surgeon. She was attentive to the clinical aspects of design to ensure what we produced was something that would be clinically useful at the end of the day.”
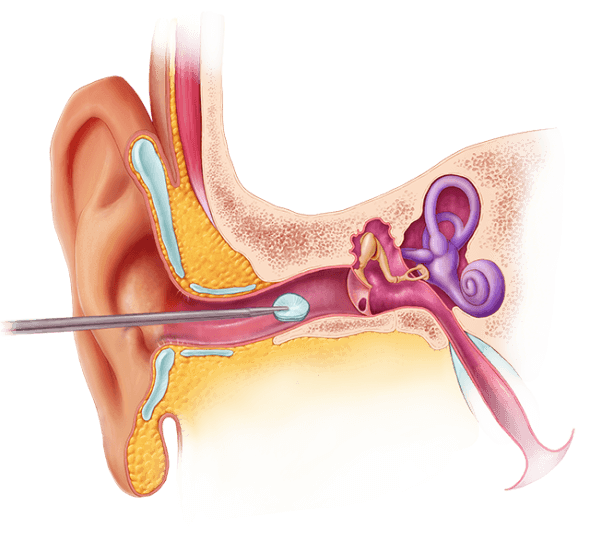
This illustration shows the noninvasive process by which the PhonoGraft is installed through the ear canal. (Illustration by Shawna R. Snyder)
Because the material is biocompatible, as the eardrum heals, native cells and blood vessels grow into the material and regenerate native tissue, Remenschneider said.
“Ultimately as these 3D-printed grafts degrade, they leave behind tissue that looks like the original 3D-printed architecture,” he said. “With biodegradation of the graft, the risk of infection in the medium- and long-term is quite low. This is a big benefit for patients.”
To help get the technology into the hands of surgeons faster, they knew they would need to launch a startup. Housed in the Harvard Innovation Labs (i-Lab), the team has benefited from fundraising advice and guidance on customer research from i-Lab experts, Black said.
As part of that customer research, they’ve been working with Harvard undergraduate students Eva Cai, S.B. ’21, a bioengineering concentrator, Juhee Goyal, A.B. ’22, an engineering sciences and integrative biology concentrator, and Marta Pawluczuk, S.B. ’22, a mechanical engineering concentrator, to conduct a survey of ear, nose, and throat doctors around the world. The students found that this technology could be especially useful in under-resourced settings. Because these grafts are designed to be placed directly through the ear canal, the less-invasive procedure is can be performed in a clinic without the need for anesthesia or an operating theatre, Remenschneider said.
In rural India, for instance, where clinicians often travel to distant communities to care for patients, this procedure could be performed without the need to bring the patient back to a hospital. Instead of two or more hours in the operating room, it can be done in 15 minutes in a clinic.
Members of the Beacon Bio team (from left) Zack Chou, Moritz Mond, Nicholas Traugutt, Sophia Smith, and Nicole Black
“Ultimately, what we are trying to do is make this procedure as accessible as possible,” Black said. “There are millions of patients worldwide who perforate their eardrum and don’t have access to a trained ear, nose and throat specialist or an operating room. What if you could repair this on the spot in a clinic setting? It’s inspiring to think that warfighters could even be treated on the battlefield, without having to wait until they return home.”
“It’s really exciting to see our technology be applied to this clinically relevant problem,” Lewis said. “Nicole’s energy and enthusiasm for this work coupled with our ability to collaborate with clinicians at MEEI has made all the difference.”
The team has secured Institute Project funding from the Wyss Institute, where they are working to de-risk the technology behind PhonoGraft. Additionally, Black was recently awarded the prestigious Lemelson-MIT Student Prize in the Graduate “Cure it!” category for the PhonoGraft invention. Harvard’s Office of Technology Development has protected the intellectual property for the novel material system and is helping the Beacon Bio team prepare for launch. Meanwhile, the research team is finalizing the design of the graft, working with regulatory experts, and collaborating with research organizations to conduct toxicity studies that would be required for FDA clearance.
For Black, who has been working on this technology since she began her graduate studies at SEAS six years ago, seeing it move toward a point where it could help patients is extremely rewarding.
Topics: Bioengineering, Entrepreneurship
Cutting-edge science delivered direct to your inbox.
Join the Harvard SEAS mailing list.
Scientist Profiles
Jennifer Lewis
Hansjorg Wyss Professor of Biologically Inspired Engineering
Press Contact
Adam Zewe | 617-496-5878 | azewe@seas.harvard.edu